
Financial stability has become a critical concern for medical practices across the board. Revenue Cycle Management (RCM) ensures that the healthcare providers are compensated fairly and efficiently for the services they provide, while minimizing revenue loss. But the question arises - how do we measure the efficiency of revenue cycle management? The answer lies in the several KPIs that can help zero in on the performance of a healthcare organization. This guide will dwell on the most important KPIs that can be tracked for the same purpose. But before we do that, let us first understand what RCM is.
What is Revenue Cycle Management (RCM)?
Revenue Cycle Management is essentially the entire financial management process from the start of the healthcare cycle to the end of it. It includes verifying patient information and helping register patient information to submission of claims, to payment processing and claim acceptance or denial.
An efficiently managed RCM process ensures that there is minimal revenue loss and delays in reimbursement. To avoid compliance or cash flow issues, it thus is imperative to track the key revenue cycle metrics to judge whether the process is functioning at its optimal level or not.
Key Revenue Cycle Metrics
Say, you have discovered that you want to make changes to your revenue cycle management. You look into the workflows, but given the enormity of the process, it becomes difficult to pin-point the issue accurately.
So what do you do?
This is where revenue cycle metrics come in handy.
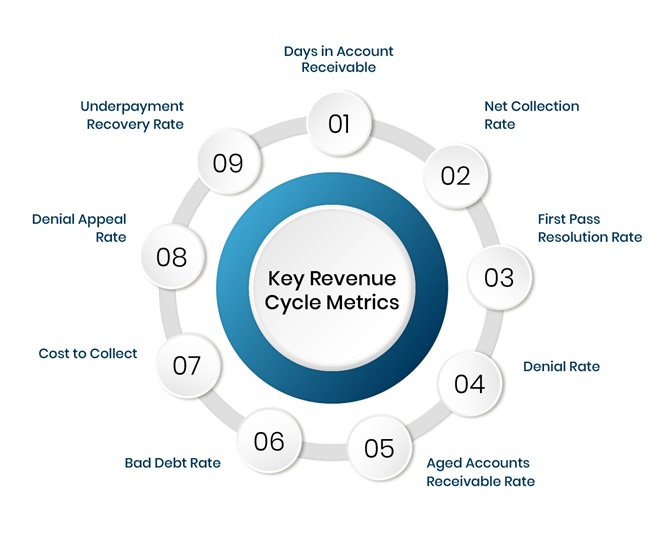
These metrics are designed to provide an informative snapshot of the entire payment cycle, for you to identify the areas of improvement. Below we list down some of the important ones for you to help navigate the cumbersome claims submission process.
Days in Account Receivable (A/R)
You may wonder why the number of days in account receivable is an informative metric for the healthcare cycle. And your question would be legitimate.
This metric computes the average time it takes for a healthcare provider to receive the payment. To put this into perspective, a lower number indicates that the process is functioning properly and the providers are getting paid in optimal time, while the higher number suggests that there are delays in payments.
The industry benchmark for this metric is 35 days, meaning that as long as the metric computes to 35 days or less, the RCM process is functioning efficiently. Several strategies can be deployed to reduce this number.
For one, it is important to simplify the claim submission process to reduce any errors that might contribute to the delay in the overall disbursement of payment. Secondly, automating patient reminders for any outstanding balance while also following up promptly for unpaid claims might help improve this metric considerably.
Net Collection Rate
How can a metric be used to identify revenue leakage? One way to judge the efficiency of the cycle is by understanding the proportion of payment collected versus the amount that was expected to be collected. This is referred to as Net Collection Rate and plays an important role in determining the overall financial health of an organization.
As long as this benchmark remains above 95%, one can safely say that the practice is financially sound and does not require any urgent intervention. The healthcare practice should ensure that regular audits of reimbursements are done so that payments are not missed. If the staff is trained on audits, many such errors in claim submission could be caught and corrected before the optimal time.
First Pass Resolution Rate
If you’re a healthcare organization, you’d want your claims to be submitted in one go. You would try to avoid the resubmission of claims due to errors. The amount of claims that do not require resubmissions can be measured using first pass resolution rate (FPRR)
A high FPRR of say 90% indicates that the cycle is running optimally and might not need an intervention. One way claims resubmission can be avoided is by implementing automation to check the claims before submission. Regular audits should be conducted to catch an error before it makes the FPRR worse.
Denial Rate
This metric measures the flip side of FPRR, which is the percentage of claims finally rejected by the payer. There could be multiple reasons why the denial rate for an organization might be high. Some of the contributing factors could be a result of bad documentation, or errors in the coding or verification process.
It is advised to maintain the denial rate below 5%.
Given the current healthcare infrastructure, sometimes maintaining it low might be hard. To circumvent this, you can try a few methods.
One thing you could do is analyse the denial trends to identify any common issue to nip it in the bud. Secondly, you can implement a real-time verification system so that no claims go to the payer unchecked.
You can check out the glossary for important healthcare terminology.
Aged Accounts Receivable Rate
The term “aged” in the metric is self-explanatory. This metric talks about the A/Rs that remains unpaid even after 90 days. Higher the number, higher the chances of issues in resolving these unpaid A/Rs.
Less than 25% of these should be aged beyond 90 days for optimal cycle.
If that’s not the case, it would be recommended to scrub the claims before submission to identify any issues beforehand. Training the staff on audit is an essential step to maintain this metric at a lower number.
Bad Debt Rate
Imagine a scenario where some of the A/Rs end up being uncollectible. This proportion of the revenue would be identified using the bad debt rate.
Rising bad debt rate is indicative of poor patient payment policies and should be redressed immediately.
The benchmark for this is pretty steep. The national average for bad debt rate for hospitals in the US is 2% - notwithstanding the reports that hospital bad debts are getting worse.
To ensure that it stays at 2% or below, it might be helpful to offer flexible payment plans to the patients or educate patients on financial responsibilities upfront.
Cost to Collect
Just maintaining the bad rate at below 2% is not enough. It is also important to keep the cost to collect at minimum to maintain profitability. This metric is essentially the total cost involved in the payment collection process.
This might include:
- Employees salaries
- Software costs
- Administrative overhead
Automating the collection process could help reduce the cost to collect, while bad debt or aged receivables could be outsourced for resolution.
Denial Appeal Rate
The utility of this metric can be demonstrated by focusing on a scenario where denied claims are repealed. The percentage of claims that manage to successfully appeal and reimburse constitutes the denial appeal rate.
There is no set benchmark for this metric.
Rates could potentially vary, but practices should aim to hit the 50% mark with this rate. This is especially in the cases where a quick correction in the original claim could resolve the issue.
Underpayment Recovery Rate
Similar to the denial appeal rate, underpayment recovery rate measures the percentage of underpayments successfully identified and resolved by the organization.
Practices should aim to recover at least 80% of the identified underpayments.
By regularly auditing payment reimbursements for discrepancies, and using the contract management software to track expected vs actual payments, the underpayment recovery rate could be significantly boosted.
Strategies to Optimise Revenue Cycle Management
Just tracking revenue cycle metrics isn’t enough.
One of the most impactful strategies for optimizing RCM is automation. Simplify tasks such as claims processing, eligibility verification, and patient billing to reduce the manual errors associated with these that cause claim denials.
Equally important is investing time in training staff. When both the front-end and back-end teams are well versed in coding, audit, and denial management, the chances of manual errors would diminish, leading to an effective RCM.
That is not to say that tracking revenue cycle metrics isn’t important in itself. It is certainly valuable when it comes to denial management, as it can help detect patterns and trends that can help avoid denials in the first place.
How Outsourcing RCM Can Improve Your KPIs
Using the insights gained from this exercise to make successful changes to the cycle is important. It’s crucial to invest in the correct technology to first enable these metrics and second, to enable the changes informed by these metrics.
Outsourcing the payment issues wherever possible could be a great strategy to navigate some of the challenges associated with maintaining a robust revenue stream.
You ask - why? For one, these are experts that simplify the entire billing and collections process, resulting in faster turnaround time and cleaner claims.
One of the most immediate benefits though is the reduction of A/R days - which is thanks to the dedicated team outsourced to follow-up on unpaid claims promptly and efficiently. Outsourcing can also lead to lower denial rates, since expert coders ensure that the claims are submitted error-free and are compliant with the regulations.
Consider partnering up with PCH Health that provides patient registration support, medical coding and audit, denial management, and revenue cycle management support. Contact us for a quick demo to understand the nitty-gritties of the product.